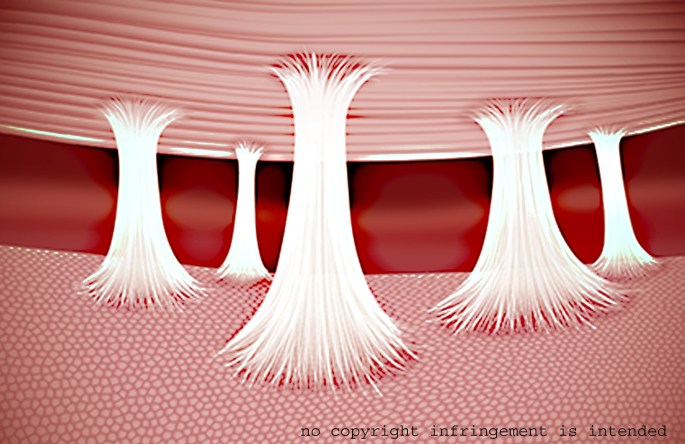
The uncommon knowledge in health-care about fibrous adhesion as a source or factor in pain leaves many patients frustrated and grasping for solutions...
Category: Assessment
I Have a Hammer so It’s a Nail
Everyone’s heard the term that if you have a hammer everything looks like a nail. This is an unfortunate reality in some aspects of healthcare.
A Missed Step in Physical Medicine
The question needs to be asked when presented with a painful condition. Is this problem associated with mechanical restrictions in the moving parts?